I write this as the US appears to be running head-first into a new wave of COVID-19 infections brought on by the rise of the Omicron variant. It is not yet 100% clear how much risk Omicron poses or how long it will be with us (though hopefully soon, I will have some thoughts on it). What is clear is new variants continue to arise because many people have no way to get vaccinated in much of the world. Omicron was first discovered in South Africa, where less than 15% of the population. Even so, South Africa is doing much better than Tanzania, which has only administered 1.7 million vaccines in a population of 59.7 million people. The longer COVID spreads amongst people without immunity globally, the larger the chance of a new variant that can keep us from moving past COVID.
Vaccine access is not a silver bullet for ending COVID; many countries still have many vaccine-hesitant people. For example, Tanzania’s former president, John Magufuli, who died earlier this year, did not believe COVID-19 was a severe threat, so the country did not try to procure vaccines during his regime. However, most of those dying from severe COVID never had a chance to be vaccinated in most low-income countries. And all indications are that vaccine hesitancy goes down in a country as people see more of their friends and family get vaccinated.
This urgent issue has renewed interest in the subject of vaccine patents and intellectual property, which pharmaceutical companies have steadfastly declined to open to the public. Countries like India and South Africa have repeatedly asked vaccine manufacturers to waive their intellectual property on vaccines. The issue became more earnest in the late spring when the Biden Administration signaled an interest in a waiver, a reversal of the traditionally strong stance the US has taken on intellectual property. There is a compelling moral intuition here: Why should profits be prioritized over the lives of vulnerable people who cannot access the vaccine? I find this intuition compelling on a basic level, but while I agree that vaccine access is a moral imperative, I do not think the policy issues here are as black and white. There are various points of complexity around vaccines and intellectual property that should be fully explored and understood before one jumps to endorsing waiving intellectual property.
Broken Vaccines Markets
It is essential to contextualize the broader state of the pharmaceutical market for vaccines. Before COVID, it would not be an exaggeration to say that vaccines were a failed market within pharma, with very little research and development creating new vaccines. Before the COVID Vaccine, we had never built a single successful vaccine for a coronavirus, including the face of the 2002 SARS and the various MERS outbreaks in the 2010s. There are many reasons for this, but it is essential to know three significant factors that make vaccines a challenging business model:
1) Any candidate vaccine may not be successful, meaning companies need to account for multiple rounds of developing the shot before it can be successfully approved. Successful pharmaceuticals indeed make absurd profit margins, but much of the “profit” on successful drugs go to recoup the losses on all the drugs that failed that were previously
2) A vaccine must go through a long and rigorous clinical trial process, which costs the companies not just money, but more importantly, time, which is often more critical in business investments (clinical trials for vaccines usually take years because you need time to ensure enough people have been exposed to the disease to prove efficacy)
3) Even if the vaccine is successful, by the time a vaccine proves effective in clinical trials, an outbreak may be over, and thus there may be no market for people willing to buy the vaccine.
Vaccines are a great example of a product with what economists call “positive externalities,” which in laymen’s terms means that they create more value for society than can be captured by the producer. Unfortunately, this factor means that free markets alone do not incentivize private actors to produce as much of these goods as society needs. This market failure is one reason governments step in with incentives for individuals who create green space on their land or an employer who does extensive job training: it is good to reward those whose actions benefit the public. While individuals should act virtuously, our society must align our policies’ incentives with virtuous action. Otherwise, we will punish those who do good while rewarding those who are selfish.
The main point here is that if the US congress functioned well to create optimal policy, the US would have long-ago acted to create a more powerful incentive for private companies to make. Instead, it took the crisis to get the US Government to invest heavily into vaccine development, which was almost certainly the best decision of our federal pandemic response. Operation Warp Speed did not have a huge budget compared to broader COVID relief: 18 billion was spent on the effort, about 0.3% of the 5 trillion spent on the pandemic relief efforts more broadly. Operation Warp Speed was also not simply a handout: it tried to address this problem at all three levels of the business model:
The US government gave upfront financing to fund the R&D stage of vaccine research. The goal was to ensure that companies would not lose their money on vaccine research if candidate vaccines did not work. Not all companies participated in these grants, notably the Pfizer vaccine (the most widely used vaccine in the US), but Moderna and other vaccines did.
The government also reviewed and cut bureaucratic red tape delays in the approval and clinical trial process that did not meaningfully ensure safety and effectiveness. This process meant companies had a reasonable assurance that they could quickly get the drug to market.
The US government also created pre-purchase agreements so that the companies knew there would be a market for the vaccines, ensuring they could ramp up manufacturing even before approval. The drug makers could assume that even if the pandemic were short-lived and demand for vaccines low, the government would honor their agreement to buy doses.
Of course, Warp Speed was, in practice, a massive windfall for the pharma companies that participated. For many progressives, this rubs them the wrong way: why should the government subsidize the profits of private companies? Most people have a moral intuition that it is morally dubious for pharma companies to profit during a pandemic. Research has found that broadly, there are many domains where people negatively react to the idea that private actors would benefit in a crisis. For example, a study by UCLA professor Paavo Monkeonen and Michael Manville showed that the most persuasive argument against building more housing in response to the housing crisis was the idea that developers would make a significant profit during a housing crisis. Specifically, they found:
“Opposition to new development increases by 20 percentage points when respondents see the argument that a developer is likely to earn a large profit from the building.”
Economist Alvin Roth, who has written extensively on markets, specifically kidney donations, calls this phenomenon “repugnant markets,” where people feel that certain business transactions are morally repugnant. Some repugnant markets are traditional vices like prostitution, drugs, and gambling. However, the intuition also kicks in when people profit from selling necessities during a crisis, including housing, food, and medicine. Therefore, many countries, including many social-democratic countries in Europe, has the government provide these goods at a low cost to the public.
I agree with the moral intuition that these necessities should be accessible to all people in a wealthy society, not just the rich. However, I want to make the case that this intuition needs to be balanced with an understanding of how markets work. Economists have long argued, maybe best by Hayek, that prices (and precisely profits) communicate vital social information. When a product reaches absurdly high prices, it signals to the rest of society that a tremendous problem needs solving! Please supply more of this as soon as possible. High housing prices should be understood as a signal of the need for more housing, and profits for developers should be seen as good if those profits go to producing something we all need.
Creating profit motivations for producing socially valuable goods in a capitalist system has historically worked well. For example, historically, the US government has heavily subsidized the solar industry in tax credits for homeowners who install panels on their roofs. These subsidies have been a wild success: by creating a profit motive, we have seen solar manufactures drive down the price to the point where Solar is now, by some measures, cheaper than coal and natural gas even without the subsidy. Solar’s development has been an incredible win for society: even if one puts aside the issue of global warming, estimates show that air pollution kills somewhere between 5 million and 10 million (high estimate) of people in the form of inducing asthma, heart attacks, and strokes. Two of the biggest culprits in this air pollution are coal-based electricity plants and internal combustion engines in gas-powered cars, technologies that solar power could render obsolete. Breakthroughs in Solar energy, driven by government subsidies and capitalist ingenuity, are hopefully getting us to a world where we could see far less pollution very soon.
The Case for Supply-Side Progressivism
Ezra Klein recently wrote an excellent article where he argued that Progressive skepticism of markets is creating a huge blind spot: the importance of what he calls “supply-side” policies. Klein writes:
Progressives are often uninterested in the creation of the goods and services they want everyone to have. This creates a problem and misses an opportunity. The problem is that if you subsidize the cost of something that there isn’t enough of, you’ll raise prices or force rationing. You can see the poisoned fruit of those mistakes in higher education and housing. But it also misses the opportunity to pull the technologies of the future progressives want into the present they inhabit. That requires a movement that takes innovation as seriously as it takes affordability.
Klein argues that the Left often makes this mistake when it comes to new drugs: the Left often looks to the stricter, like Europe is in regulating drug prices, arguing that the current patent regime in the US is too friendly to pharma companies. And while Klein is sympathetic to this line of thought, he wants to make sure the Left does not overlook the importance of incentivizing new drug development:
Americans overpay compared to peer countries for drugs. But truly curing, managing or preventing disease is of extraordinary value to humanity. Pfizer and Moderna will make billions from their coronavirus vaccines, but they’ve created trillions of dollars in economic value by unfreezing economies, to say nothing of the lives saved. It is true that European countries free-ride off the high cost we pay for drugs, because it’s the U.S. market that drives innovation. But that doesn’t mean we’d be better off paying their prices, if that meant new drug development slowed. We don’t just want everyone to have health insurance in the future. We want them to be healthier, freed from diseases and pain that even the best health insurance today cannot cure or ease.
This dynamic played itself out when it came to vaccines. The US did not get early access to vaccines simply because of wealth; other wealthy countries got access to vaccines much later. A significant factor was that the US was willing to enter into relatively generous pre-purchase agreements with pharmaceutical companies. At the same time, the EU took a harder line, trying to negotiate a lower price with the vaccine makers. By the time Europe negotiated the price low enough, the US, UK, and Israel had already gotten in the front of the vaccine line. Wealthy Left-Wing countries were not the only ones whose hardline tact misfired. Under Modi’s current economic nationalist vision, India declined to buy vaccines from the US companies because they wanted to produce their vaccine locally.
I want to be very careful here: I am not saying the US deserved the vaccine or that other country’s failure to act means they don’t earn access. Instead, it is to make the point that when it comes to innovation, it is easy to miss the forest from the trees: the amount of profit that vaccine manufacturers are making pales in comparison to the lives they are saving. We will never know with precision how many deaths vaccines saved, but one recent study that tried to quantify the value argued vaccines saved 1.1 million lives in the US in 2021. Suppose you take the US government’s official value of a statistical life (7 million dollars per life). In that case, that means that vaccines created 7 trillion dollars in economic value in the USA alone, 200 times more than the $34 billion in profits that Pfizer, BioNTech, and Moderna will make in 2021. The instinct to draw a hard line that companies make “too much” profit (or that only domestic companies can profit) runs the risk of eliminating the incentive we need for innovation. The impact of less innovation not only hurts society as a whole, but it harms the most vulnerable, who are often most exposed to the harms of the status quo. My neighborhood of East LA was disproportionately harmed by COVID-19 and is still disproportionately harmed by the air pollution produced by the many freeways that go through our community. A world without vaccines or solar power is one where we are far worse off as a neighborhood.
I see this argument a lot in the housing policy space about an idea called “value capture.” Because of how restrictive our current zoning codes are, many new housing developments require city planning officials to grant them special permission to build above the current zoning limit. This permission could look like asking to construct an 8-unit apartment building in a zone where only single-family homes are legal or a 20 unit building in an area where only four are legal. Value capture is the idea, most strongly held among progressive planners, that allowing these zoning variances to developers is essentially a “handout” because the land value will skyrocket once a 20-unit building is approved. Thus, value capture argues that some of the value created by the zoning change needs to be “captured” by society, usually in the form of affordability requirements in the new project.
I am not opposed to the idea of value capture in theory; however, I worry that how value capture is practiced is counterproductive (as UCLA professor Michael Manville argues). In the middle of a housing crisis, trying to take a hard line and extract value from developers often does diminish the amount of new housing built. There is no calculation in the value capture framework because new housing does provide public benefits by being built: research shows that new (“luxury”) housing drives down rents both city-wide and in the local neighborhood around the site. Value capture is only ever applied to new development: no efforts are made to capture the appreciation of single family homeowners who have done nothing to add to their house, yet whose houses have appreciated by hundreds of thousands of dollars. I sometimes joke about what this would look like:

Furthermore, research shows governments will set the value capture at too high a rate. Frequently, you get more affordable units when you place a value capture at a small percentage, which incentivizes more projects to become feasible and can lead to a higher number of affordable units produced at a city-wide level. Without a profitable business model, developers will not build housing. Theoretical affordable projects that are never feasible enough to be created in real life do not help real people.
So yes, you can make a case that the design of Operation Warp Speed created a lot of value for pharma companies. But that does not necessarily make it wise to try to “capture” all of that value; vaccines have created far more value for the general public than for Pfizer and Moderna. Misapplying this mental framework of value capture risks undermining innovation altogether.
So…What do we do about Patents?
All of that said, my argument is not that we should dismiss the urgency of vaccinating more people. Instead, we need to see this as an issue where we must hold the tension of caring about universal access AND future incentives. And while I worry that Progressives who want to waive patents without an alternative are not maintaining this tension sufficiently, I also do not think the current patent legal regime in the US is the best policy approach. As I discussed earlier, the vaccine market pre-COVID was not working; even with the expectation of robust patent protection, vaccine makers were still not producing vaccines at a high rate.
In many ways, patents are not an ideal system. Researching new medicine costs a lot of money; manufacturing medicine often costs a fraction of the research costs. Patents create a system where drug makers expect to charge a price that covers the research costs and then returns a profit. It only works because patents grant an artificial monopoly: they prevent other companies (who did not do the research) from simply charging a minuscule price for a generic version of the drug, competing down the price in the marketplace. As a result, patents often mean that drug markets have artificially high prices and an artificially low supply. Patents can create an incentive to innovation, but they also can create an incentive to abuse the system. This incentive is especially true because the actual price of drugs is often obfuscated as they are paid for by third parties, including both the government and employers through insurance companies.
Brink Lindsey, who wrote more extensively about issues of intellectual property in his book The Captured Economy, wrote about some of the flaws of the patent system:
the U.S. patent system at present is out of balance. Over the past few decades, the expansion of patentability to include software and business methods as well as a general relaxation of patenting requirements have led to wildly excessive growth in these temporary monopolies: the number of patents granted annually has skyrocketed roughly fivefold since the early 1980s.
One of the worst abuses are those of patent trolls:
One unfortunate result has been the rise of “non-practicing entities,” better known as patent trolls: firms that make nothing themselves but buy up patent portfolios and monetize them through aggressive litigation. As a result, a law that is supposed to encourage innovation has turned into a legal minefield for many would-be innovators.
And the Pharma industry is a terrible actor here:
In the pharmaceutical industry, firms have abused the law by piling up patents for trivial, therapeutically irrelevant “innovations” that allow them to extend their monopolies and keep raising prices long beyond the statutorily contemplated 20 years.
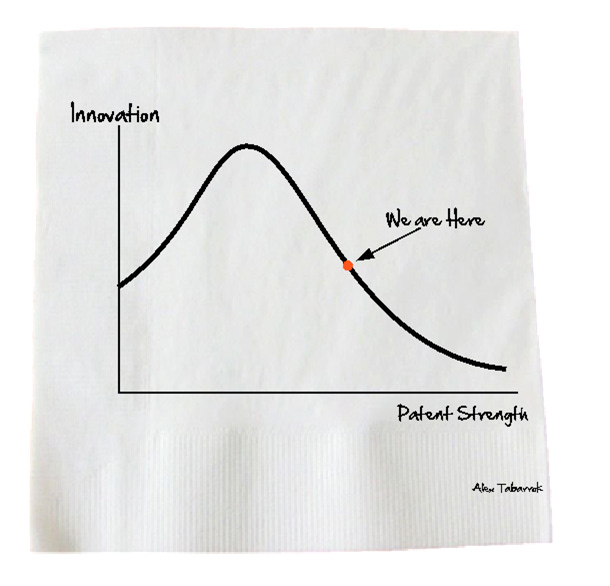
Alex Tabarrok, who is a right-of-center Economist, tried to illustrate the problems with IP law back in 2012:
Tabarrok’s point was to illustrate the trade-off between innovation and patent strength as a curve with a point where you can maximize innovation with patent protection. The problem, as he explains, is that research shows we are almost certainly too far in the direction of patent protection.
So while it is true that many of those who critique patents do not take the problem of incentives seriously, it is also true that defenders of patents do not fully reckon with their limitations. For patents to work as an incentive for innovation in drug development, two things must be true:
There must be a reasonable chance of the pharma research and development to lead to a drug that can be approved successfully
There must be a significant assurance that a market for the drug will exist far enough into the future that
As previously discussed, creating vaccines in response to novel pandemics hardly ever neatly fits these two criteria. Moreover, it is impossible to tell at the outset if a pandemic will burn out quickly or linger for years, and it is hard to predict whether new technology will work in the face of a new pandemic.
However, the success of the COVID-vaccines has led to a burgeoning investment in this area. For example, a malaria vaccine in development would be a game-changer in sub-Saharan Africa, where hundreds of thousands of lives are lost every year to malaria. Likewise, there is a pan-coronavirus vaccine in development that, if successful, could not only help protect against all future COVID variants but also against future pandemics and even coronaviruses that circulate as “common colds.” Changes in our policy approach to patents should incentivize MORE of these moonshot biotech projects, not less. One must weigh the lives that a patent waiver would save against lives that may be lost in future pandemics if taking away patents decreases the speed of response by pharma companies.
And this is where we should be honest that there is significant uncertainty that opening up the vaccines patents may not expand access. Pfizer and Moderna have not been acting in a textbook monopolistic fashion; instead, they have been aggressive in building out a network of partner manufacturers to whom they can transfer their vaccine technology. Recently they announced expansions through partners in South Africa and South Korea, countries that previously struggled to access vaccines. In addition, companies have priced vaccines relatively modestly: the US government has paid Moderna between $32 and $37 a dose, which is a small amount compared to the price of insulin, which can run between $100 and $400 a vial.
Vaccine companies claim that the most significant reasons manufacturing capacity are limited are supply chain issues and lack of suitable global manufacturing facilities. As companies have scaled up vaccine production, there have been shortages in many parts of the supply chain: from plastic bags to Chilean Tree Bark. Vaccines companies have argued that if you open patents up, there will be too much competition for those precious inputs, and no one will be able to get doses out fast enough. There are reasons to take these claims seriously: vaccines, unlike many prescription drugs, are quite a complex manufacturing process:
Years ago, Tesla opened its patents on its battery technology and said it would not enforce those who copied them. Tesla had a specific business reason to do this: they were hoping that putting their technology out in the open would help kickstart more electric car manufacturing and, thus, more infrastructure buildout to make electric car ownership more feasible. No one would argue that opening this battery technology has precisely led to a proliferation of copy-cat Teslas hitting the market.
Before I start to sound like a shill, I think it is vital to hold skepticism towards the vaccine makers since keeping their patent is in their self-interest. Markets have a way of inspiring creativity and proving wrong those who think that resources are fixed. Let us look no further than early in the pandemic when public health agencies assumed we had a fixed supply of masks. Thus, telling people to mask was counterproductive as it would diverge resources away from medical personnel. Instead, once people realized that simple cloth masks could be helpful, we saw the rapid proliferation of people manufacturing imperfect yet still better than nothing cotton masks around the globe. It seems clear that the only way to know whether patents are a problem in this space would be to remove the patent and see if people can step up to the plate and manufacture new vaccine doses, even if that process would certainly take months to get up and to run.
But our goal should not be to remove patent protection; we need to make sure that we replace it with a guarantee that can align the incentives of pharma companies with the global public good. The best proposal I have seen for this is one of the prizes. This system has been supported broadly in the past, from everyone from the Libertarian Cato institute to Bernie Sanders, who proposed a prize system years ago in congress.
The details here would be simple in theory: under the prize system, the US government could simultaneously make patents less lucrative (by limiting their scope and years) and create conditional prizes to buy out patents of drugs once developed. Then, once a manufacturer can demonstrate efficacy, the government would pay a lump sum to buy the patent and a public release of any necessary technical knowledge needed to produce the product. Companies could then compete in manufacturing the product as a generic, creating lower drug prices for consumers. This system would look much more like a traditional free market than the current system and help start to make significant inroads in reducing the extremely high costs of US healthcare.
Setting the right monetary prize for new drugs would be tricky, and there is no reason to think that governments would get it 100% right. There would almost certainly be pressure to give prizes lower than ideal, given that taxpayer dollars are at stake. However, a relevant agency could not layout criteria to approximate what prize amounts should be. We could start by looking at the size of the market need, the lethality of the condition, and the product’s effectiveness. Those skeptical are also worth noting that the current system of funding medical research in the US has its own set of problems through the NIH. The NIH grant process is extremely burdensome, and grants only have a slight chance of success (around 10%) while tending to go only to the most senior scientists. A prize system would give younger, less well-connected researchers a chance to break through and hopefully allocate resources and research towards higher value purposes.
In the case of the COVID patents, we are too late in the process for a buyout to do the maximum possible good, given that we are almost one year into the vaccine rollout. But given that many countries are still waiting for vaccines and there is increasing reason to think vaccines may need to be periodic in the most vulnerable people, it still may have merit. If governments worldwide want to ensure vaccines are as cheaply accessible as possible, they should band together to offer the vaccine companies couldn’t refuse. Would offering 50 billion to buy out the three patents be outrageous, considering the tens of trillions of dollars of relief that rich governments have spent during the pandemic? To me, setting aside money for a patent buyout looks quite reasonable. There is no such thing as an easy fix to a complex problem: if we want to do good for the vulnerable in the long and short-run, we should be willing to commit resources to the cause. And while this may not be as politically popular as sticking it to big pharma, I do think it is a far more responsible policy approach.